A patient portal only works if patients trust it. Once that trust is broken, organisations rarely get a clean second chance to rebuild it. Most of the decisions that determine whether trust holds are made at the portal layer: what data is shown, when, to whom, and how each of those choices is explained. They sound like UX questions, but they aren’t really. They’re clinical, legal, and architectural, and they carry weight well beyond the design system.
The Architecture Behind the Record
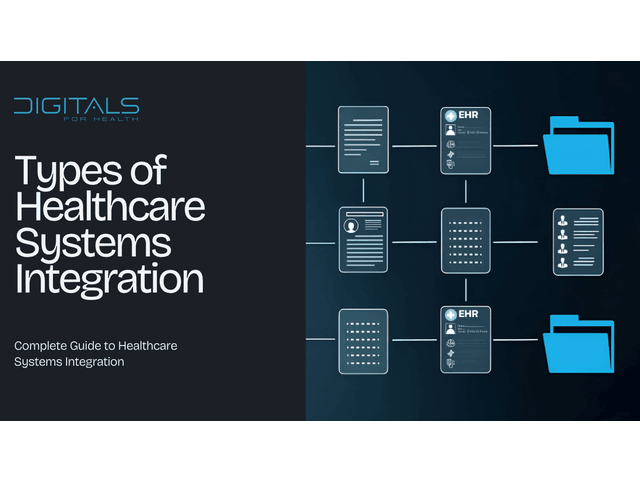
A patient portal typically surfaces test results, treatment plans, appointment history, medication records, and messaging with the care team. Almost none of that data lives in the portal itself. Instead, the portal acts as a presentation layer, pulling from systems sitting elsewhere: a LIMS for lab results, an EPR prescribing module for medications, a scheduling platform for appointments, and a document store for anything that doesn’t fit neatly into structured data. Each of those systems has its own authentication model, schema, and latency profile.
To the patient, all of this should look like a single coherent record. Making it look that way reliably requires event-driven synchronisation rather than batch processing. A result filed in the lab system needs to appear in the portal within seconds, not on the next overnight cycle. Publish-subscribe is the pattern that holds up here. Source systems emit change events to a message broker. An aggregation service consumes those events and maintains a read-optimised projection. The portal queries the projection rather than hammering backend systems on every page load.
See also: Integration is where the NHS 10 Year Plan lives or dies → on the interoperability challenges, legacy systems, and clinical safety considerations that sit underneath every patient-facing integration.
Making the Data Safe to Show
Where FHIR R4 APIs exist at the source, the portal fetches data using standardised resource types: DiagnosticReport for lab results, MedicationRequest for prescriptions, Appointment for scheduling, and AllergyIntolerance for safety-critical records that cannot tolerate incompleteness. Where FHIR isn’t available, a translation layer normalises proprietary formats into a canonical model before anything reaches the patient. Field-level validation then catches truncation and encoding errors early. Before they surface as something a clinician has to explain in the room.
Results release is the part that always comes back in a workshop. A result arriving from the LIMS should not go straight to the patient. Instead, it passes through a configurable hold workflow where a clinician can review and release it with appropriate context. Hold duration and release conditions are configurable by result type, abnormality flag, and urgency. Crucially, the hold state lives in the aggregation layer rather than the source system. That means the LIMS needs no modification, and the rules can evolve as clinical practice changes.
Pipeline health belongs in the observability stack alongside uptime and response time. Event lag, failed deliveries, and dead-letter queue depth all need to be visible. A portal that silently stops receiving updates will go on showing patients a stale record with no indication that anything is wrong, which is one of the worst failure modes available in this space.
Transparency in Data Usage
Under UK GDPR, patients have a right to know what data is held about them, why it’s being processed, who it’s shared with, and how long it’s kept. Most organisations treat that as a documentation problem and write a privacy notice. A more honest approach surfaces it in the product itself.
In practice, that means access logs showing patients which practitioners viewed their record, when, and from which organisation. It also means consent notices written in plain language and presented at the moment a processing decision is being made. Not buried in a sign-up flow nobody reads. Beyond that, it means controls that let patients hold separate preferences for direct care, anonymised analytics, and identifiable research. Most patients feel quite differently about those three things, even when the legal text bundles them together.
The infrastructure underneath this is a dedicated consent service that stores records against specific processing purposes and data categories. Eeach with a timestamp, a version identifier, and a record of how consent was given or withdrawn. Rather than checking consent at login, a policy enforcement point between the API gateway and the backend data sources evaluates it on every request. Policies are declared against consent state and role context, evaluated dynamically, with decision logs that can be independently audited for data subject access requests.
Proxy access is where the access model gets tested. A carer, a parent, or a support worker acting on behalf of a patient needs a clearly bounded view of the record. OAuth 2.0 scopes and SMART on FHIR launch context enforce those boundaries at the API level. A delegated user can book appointments without being able to read clinical notes. The delegation itself carries an explicit scope, a consent record, and an expiry. Revoking a delegation takes effect on the next token validation, not the next login, which sounds like a small detail until you need it.
Where Trust Breaks
Most trust failures in patient portals don’t come from breaches. They come from things that feel unexplained.
A message sent through the portal that disappears for a week. A consent preference set last year that seems to have changed without notice. An error screen that says something has gone wrong, with no indication of what the patient should do next. None of these are technical failures in the strict sense. Even so, each one quietly erodes the patient’s confidence that the system is working in their interests.
Secure messaging needs SLA enforcement at the infrastructure level. Each inbound message should generate a timestamped task in the clinical workflow system. Its status (received, assigned, responded) should be visible to the patient back in the portal. Consent migration, when it has to happen, should be treated as a formal data process: preferences mapped explicitly to the new schema, patients notified of any change, a reconciliation report produced for audit. API errors need structure too. An error code that distinguishes a backend timeout from a permissions failure from a validation error, a human-readable explanation written for the patient rather than the developer, and a next step rather than a dead end.
Our Expertise
We design and build the digital front door: portals that give patients round-the-clock access to their own care. With the level of transparency and control that the regulation now expects and that patients are starting to expect alongside it.
In practice, that means secure access to test results, treatment plans, and medical history; GDPR-compliant messaging between patients and providers; online appointment booking against real-time availability; digital prescription requests integrated with pharmacy systems; and automated reminders for appointments, medication, and preventive care. Everything is built mobile-first, with accessibility and compliance designed in from the start rather than retrofitted later.